 Erick was born at the Cherese Mari Laulhere BirthCare Center at Miller Children’s & Women’s Hospital Long Beach and was then rushed to the Neonatal Intensive Care Unit (NICU) because he was born with a cleft lip and palate, a congenital defect where there is an opening or split in the upper lip and roof of the mouth or both. His condition led to his first surgery at Miller Children's & Women's Surgical Center to repair his palate at only 6 months old.
Erick was born at the Cherese Mari Laulhere BirthCare Center at Miller Children’s & Women’s Hospital Long Beach and was then rushed to the Neonatal Intensive Care Unit (NICU) because he was born with a cleft lip and palate, a congenital defect where there is an opening or split in the upper lip and roof of the mouth or both. His condition led to his first surgery at Miller Children's & Women's Surgical Center to repair his palate at only 6 months old.
A cleft lip and cleft palate can create speech difficulties, voice impairments, feeding difficulties, and other symptoms. The condition also can result in difficulty creating certain sounds, which makes it difficult for others to understand when communicating. Therefore, two surgeries are sometimes needed in order to help speech develop properly.
“About 20% of children who have a history of cleft lip and palate will need a secondary surgery to their palate. This is because the palate is either too short or it’s not moving the way it’s supposed to,” said Suki Miceli, speech language pathologist at Cherese Mari Laulhere Children’s Village.
In order to further improve his speech capabilities, Erick was referred to the Craniofacial Center at the Stramski Children’s Developmental Center for his second round of facial repairs. The Craniofacial Program at the Stramski Center is a California Children’s Services (CCS) approved Special Care Center (SCC). This means a specially designated multi-disciplinary care team is responsible for all care coordination and case management of a patient in this program. Patients typically qualify for the Craniofacial CCS Special Care Center by medical diagnosis, complexity of their disease and financial status.
The Craniofacial Program provides care to children with congenital birth defects such as cleft lip/palate, skull or ear problems and other craniofacial abnormalities. Treatment is determined by not just one doctor, but a multi-disciplinary team of specialists consisting of a plastic/craniofacial surgeon, neurosurgeon, pediatric dentist, orthodontist, oral surgeon, speech language pathologist, nurse specialists and social worker.
“Erick is a fighter. He has been a trooper throughout the entire process. Even after his second surgery for the pharyngeal flap, he recovered quickly and was back to being an active 8-year-old,” says Maira, Erick’s mother.
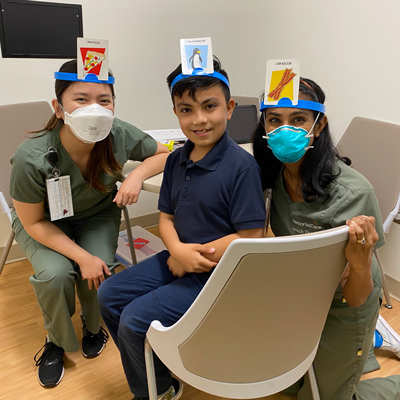
To continue to help Erick improve in his speech development, he attends speech therapy regularly at the Children’s Village. He looks forward to his sessions once a week and enjoys participating with his speech therapist.
“Since his second surgery, Erick has improved immensely. The surgery gave him the structure of his palate that he needed to be able to articulate his words more effectively,” says Suki.
The speech language pathologist aims to maximize a child’s communication and ability to understand information, while ensuring safety while eating and drinking, as well as educating family and community members how to best support the child.
“I have seen big improvements, not just as his mother, but our extended family notices it too. They notice that they can understand him substantially better when he communicates,” says Maira.
Erick’s speech pathologist has now been focused specifically on the improvement of his sounds; he can now make p’s, b’s, t’s, d’s, and s sounds, and is currently working on his L’s. Erick’s strength and efforts after going through multiple surgeries and speech therapy sessions continue to inspire his care teams at Miller Children’s & Women’s.
To further support patients, speech-language pathologists at Miller Children’s frequently collaborate with local school districts, medical providers and other therapies — occupational, physical and recreational — to continue to improve the functioning of their patients at home, in school and in the community.
Learn more about the Craniofacial Center.

