Cardiac catheterization is a procedure used to diagnose and treat various heart problems in children. While a diagnostic cardiac catheterization is used to help identify a heart problem, an interventional catheterization is used to treat the condition. In some cases an open heart operation can be avoided, while in other cases it is done to help improve the success of the surgery. We have a state-of-the-art cardiac catheterization laboratory (see more information on this page) and a specially trained staff of nurses and technologists. The cardiac catheterization laboratory includes bi-plane imaging, which allows doctors to visually follow the path of blood flow through imaging technology to create a "roadmap" for treating each patient's unique condition. The heart of an infant can be as small as a walnut, so bi-plane imaging is especially helpful in determining the best treatment for such a tiny heart. Our specially trained pediatric cardiologist performs the cardiac catheterization by advancing plastic tubes (catheters) through blood vessels to the heart, while the child is asleep (under anesthesia). This is done under X-ray guidance in the cardiac catheterization laboratory, with all of the specialized equipment needed to diagnose and treat heart problems in children.
Atrial Septal Defect (ASD) Closure
An ASD is a hole between the upper chambers (right and left atrium) of the heart. With an ASD, blood flows through the septal defect from the left side of the heart to the right side of the heart, resulting in extra blood flow to the lungs. Over many years, this can result in high pressure in the lungs and extra work on the heart, as well as heart rhythm problems. Several different devices are available that can be used to close an ASD.
Ventricular Septal Defect (VSD) Closure
A VSD is a hole between the lower pumping chambers (right and left ventricle) of the heart. With a VSD, blood flows through the septal defect from the left side of the heart to the right side of the heart, resulting in extra blood flow to the lungs. This may result in poor growth in infancy, as well as long term problems with the heart and lungs. Some specific types of VSDs can be closed with devices, while others require cardiac surgery to repair.
Patent Ductus Arteriosus (PDA) Closure
In some babies and children, a blood vessel known as the ductus arteriosus fails to close normally after birth. This condition, known as patent ductus arteriosus, allows blood from the main artery leaving the heart (aorta) to flow back into the main blood vessel to the lungs (pulmonary artery), which may place the heart under added strain. In many babies and children, this condition can be corrected by placing device into the PDA to stop the abnormal blood flow.
Balloon Valvuloplasty
A narrowed heart valve may cause extra work for the heart and lead to long term damage. Specialized balloon catheters can be used to open these narrowed valves. This minimally invasive procedure is considered the treatment of choice for many patients with congenital stenosis (narrowing) of the pulmonary and aortic valves.
Balloon Angioplasty and Stent Placement
A balloon angioplasty is a procedure to dilate (open up) a narrow blood vessel, such as the aorta supplying the body or the pulmonary artery supplying the lungs. Sometimes balloon angioplasty is not able to open a narrowed blood vessel sufficiently and your child’s cardiologist may decide that placing a stent will have a better result. A stent is a metal tube made of a wire mesh that is placed onto a balloon catheter. When the balloon is inflated, the stent expands, and is then left in place while the balloon catheter is removed.
Coil Embolization
Abnormal blood vessels (collaterals) may form in some types of congenital heart disease, which may lead to lower oxygen levels or extra work on the heart. Embolization allows precise occlusion (blocking) of these extra collateral vessels using various coils or other devices.
Transcatheter valves
Some forms of heart disease involve narrowed or leaky heart valves that need to be replaced. While this was previously done exclusively with open heart surgery, in some patients this may be performed using cardiac catheterization through the vein in the leg.
The heart has its own electrical system to regulate how fast or slow the heart beats. In some children, an abnormal heart electrical system can cause problems with the heart rhythm (too fast or too slow), resulting in feeling tired, dizzy, fainting, or even more serious problems. We can perform highly specialized electrophysiology (EP) catheterizations to treat abnormal heart rhythms. Some kinds of EP catheterizations are:
Electrophysiology Study (EP study)
When the heart’s electrical system is abnormal and causes abnormal heart rhythms, the first stage of repairing the abnormal heart rhythm isto identify the origin of the abnormal rhythm. After the child is asleep, the pediatric cardiologist places several soft plastic tubes (catheters) into the groin (top of the leg) and advances the catheters carefully into the heart to record the electrical heart rhythm impulses, creating a map of the electrical system.
Ablation
During the same procedure as mapping the abnormal electrical system (EP study), special catheters may be positioned where the abnormal electrical impulses are located, and either heat (radiofrequency ablation) or cold (cryoablation) are directed at these locations to repair the abnormal electrical system. Ablation is most often done for children who have episodes of a rapid heart rhythm called supraventricular tachycardia (SVT), as well as other forms of abnormal rapid heart rhythms.
Pacemakers
Some types of abnormal heart rhythms are too slow, and children sometimes need to have a permanent pacemaker placed in order to regulate the heart rhythm. A permanent pacemaker is a small box about the size of a silver dollar that is placed under the skin and muscle. The pacemaker delivers electrical impulses to control the heart rhythm (much like the heart’s normal electrical system) through one or more leads, or thin wires that are placed into the heart through a vein.
Automated Internal Cardioverter-Defibrillator (AICD)
Although uncommon, some kinds of abnormal heart rhythms can be life-threatening and require an electrical shock to restore the heart rhythm to normal. Some of these life-threatening heart rhythm problems are inherited, or run in families. An AICD is a special type of pacemaker that can detect these life-threatening heart rhythm problems and deliver an electrical shock to treat the abnormal heart rhythm and prevent cardiac arrest.
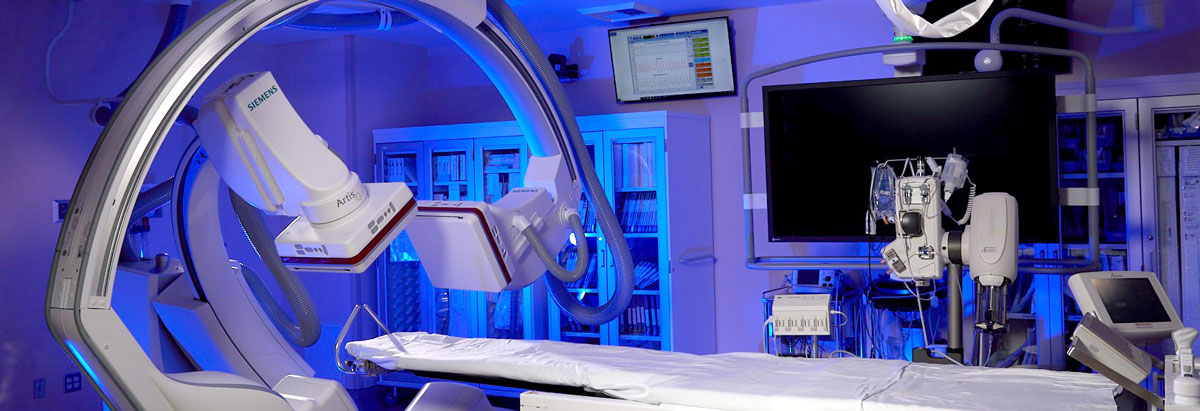
We have a suite of five cardiac catheterization laboratories, which are examination rooms with diagnostic imaging equipment used to visualize the chambers and arteries of the heart to treat abnormalities. One of our catheterization laboratories includes bi-plane imaging, which is especially helpful in diagnosing and treating children.
Bi-plane imaging, which allows doctors to follow the path of blood flow through the vessels to create a "roadmap" for treating each patient's unique condition. The digital x-ray technology uses two mounted rotating cameras, one on each side of the child, to take simultaneous pictures. The two sets of images are brought together on a computer screen to form a 3-D portrait of the heart.
The advanced technology and imaging helps pediatric cardiologists better visualize the heart and create a 3-D image. This greatly enhances their ability to perform interventions on children using balloons, stents and specialized catheters to correct congenital or acquired heart defects. The image we are able to produce allows us to print a 3-D version of the heart, so we can determine the best treatment option for each individual child.
Even though the cardiac catheterization laboratories are located in Long Beach Medical Center, the pediatric team is with you and your child every step of the way. Even your child’s anesthesiologist is board-certified in pediatric anesthesiology. Child Life Specialists also are available to help lessen any anxieties your child may be experiencing.
Depending on your child’s age there are different ways to prepare them for a heart catheterization procedure in the catheterization lab. Even though it may seem scary, explaining what is happening to your child at a young age can help them feel more at ease and not be so scared when they get to the hospital.
- Infants and toddlers should bring their favorite blanket, stuffed animal, or pacifier to make them feel more at ease and relaxed.
- Preschoolers may enjoy watching their favorite video or reading book. It may be good to tell your preschoolers a few days before the heart catheterization.
- Older children can bring in their favorite music to make them feel more at ease. Older children may have questions of their own and parents should answer their questions honestly.
Morning of the Procedure
- Your child should not eat or drink anything the morning of the procedure.
- Your child will get anesthesia (medicine to put your child to sleep) to make them sleepy and relaxed about 20 minutes before the heart catheterization.
- You can stay with your child until it’s time to perform the heart catheterization.
How is a heart catheterization performed?
- Your child will lie on an exam table that has an X-ray machine over it.
- Your child will have his/her heart rate, blood pressure and oxygen levels carefully monitored by a skilled catheterization lab team.
- Once the catheter gets to the heart, contrast (dye) will be injected to see where the heart defect is, so the pediatric cardiologist can repair it. Your child will feel a little warm for a few seconds, during the time the contrast is injected, like drinking hot chocolate fast.
What happens after the heart catheterization procedure?
- The catheter will be removed and a bandage will cover your child’s leg where the catheter was put in. Your child will need to keep his/her leg straight for a few hours to decrease bleeding.
- Your child will be taken to the PICU, where he/she will be monitored. During this time your child will need to be quiet and lay flat.
- Your child’s nurse will monitor the pulses, skin temperature and any bleeding in the leg that was used for the test.
- The length of time it takes for your child to wake up varies for each child and the type of medicine given during the catheterization.
- When your child is awake, he/she may drink clear liquids. If this happens without a problem, then your child will be placed on a normal diet.
- Your child will be discharged from the hospital, once he/she does not require further monitoring. Instructions for home care of the catheterization site will be given upon discharge.