When thinking of a stroke patient, most people think of an older adult or someone who has pre-existing medical conditions. What most people don’t know is that strokes affect people of all ages, even young children and infants. Strokes are one of the top 10 causes of death in children under 18 in the United States, and strokes in children most often occur within the first month after birth.
Recently, the Cherese Mari Laulhere Pediatric Intensive Care Unit (PICU) at MemorialCare Miller Children’s & Women’s Hospital Long Beach, in collaboration with the Comprehensive Stroke Center at MemorialCare Long Beach Medical Center, implemented telemedicine technology to quickly diagnose a stroke in a pediatric patient – one of the benefits of two full service children’s and adult hospitals sharing a medical campus. Miller Children’s & Women’s is one of a few children’s hospitals that uses telemedicine technology specifically for strokes.

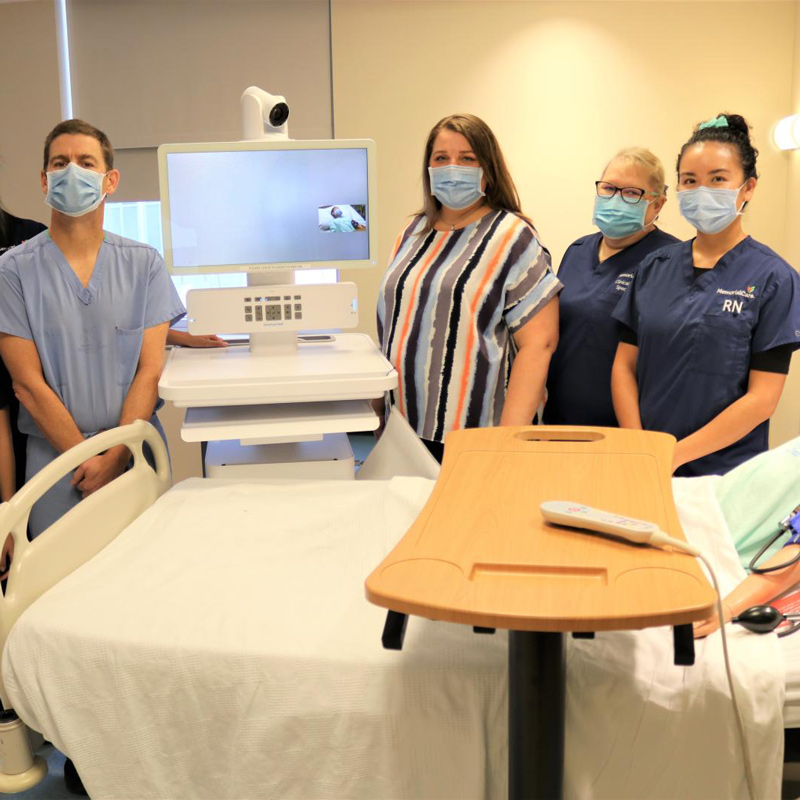
Using a “telemedicine cart” located in the PICU, specially trained pediatric neurologists can assess a patient no matter where they are by using a camera located on the cart. The neurologist can control the camera and zoom in to see the patient from a cell phone, tablet or other device, to visualize symptoms, while communicating with the onsite team to quickly determine next steps.
The fully-mobile cart is used for patients both in the PICU and patients arriving to the Emergency Department. Should a stroke be suspected from any area of the hospital, a team of response nurses trained to assess strokes in children and respond to other emergent situations will bring the cart to the child to perform the rapid assessment.
As with adults, a stroke can be life threatening if not treated quickly. That’s why it’s critical that a stroke is assessed immediately, so treatment can begin as soon as possible.

However, diagnosing strokes in children is much more difficult than in adults. In pediatric patients, stroke symptoms can be similar to other health issues that occur, such as a migraine or the flu. It also is harder for younger children to explain exactly what they’re feeling. And because strokes are uncommon in children, parents don’t suspect their child is suffering from one and may delay seeking medical attention.
Thankfully, the same life-saving acronym used to identify a stroke in an adult also can be used for children. You can recognize the signs of stroke with B.E. F.A.S.T. It stands for balance lost, eyes blur, facial drooping, arm weakness, speech difficulty and time to call 911.
“With our increased education on pediatric stroke care and implementation of stroke telemedicine technology, our patients are quickly and appropriately diagnosed 24/7,” says Christopher Babbitt, M.D., medical director, Pediatric Intensive Care Unit, Miller Children’s & Women’s. “Our highly-specialized pediatric neurologists and nurses help ensure the best possible outcomes for our youngest stroke patients.”